New guidelines released November 16, 2009 by the U.S. Preventive Services Task Force call for less mammography screening to spare women some of the worry and expense of extra tests to distinguish between cancer and harmless lumps. That’s a good call. The Task Force said:
“USPSTF recommends against routine screening mammography in women aged 40 to 49 years. The decision to start regular, biennial screening mammography before the age of 50 years should be an individual one and take patient context into account, including the patient’s values regarding specific benefits and harms.”
The Task Force said the modest benefit of mammograms must be weighed against the harms – false positives, overtreatment, and radiation exposure. Despite all the studies, it is inconclusive that bi-annual mammograms begun at 40 result in any benefit. Some lives are saved by early detection while many more may be damaged by biopsies and medical intervention applied to tumors that otherwise would disappear spontaneously. About three-quarters of the biopsies turn out to be benign, so three out of four women endure the fear that they have breast cancer – which is no small fear.[1]
It is not the first time we have heard a recommendation to back off mammograms for women in their 40s. In early 2007, the American College of Physicians said women in their 40s should talk to their doctors first about the pros and cons of mammograms.
No other country in the world recommends regular mammograms for women in their 40s.
The Radiation Factor
According to the National Cancer Institute, “most cancers come from random mutations that develop in body cells during one’s lifetime – either as a mistake when cells are going through cell division or in response to injuries from environmental agents such as radiation or chemicals.”[2]
Mammography represents frequent exposure to ionizing radiation. Radiation accumulates in the body. The only acknowledged cause of cancer by the American Cancer Society (ACS) is radiation. Yet the ACS urges premenopausal women to get mammograms even though evidence suggests that premenopausal women are more sensitive to cancer risks from radiation. No nation other than the U.S. routinely screens pre-menopausal women by mammography.
Dr. John W. Gofman, an authority on the health effects of ionizing radiation, estimates that 75 percent of breast cancer could be prevented by avoiding or minimizing exposure to the ionizing radiation. This includes mammography, x-rays and other medical and dental sources.[3]
Low-dose radiation from mammograms and chest X-rays may increase the risk of breast cancer in young women who are already at high risk because of family history or genetic susceptibility, according to a study released in November, 2009. Pooling data that involved 12,000 high-risk women from Europe and the United States, the team found that of the 8,500 women who had been exposed to radiation from chest X-rays or mammograms before the age of 20, or those who had had five or more exposures, were 2.5 times more likely to develop breast cancer than other high-risk women who had not been exposed.[4]
The timing of exposure can be as important as the dose. Younger women are at a higher risk from radiation than are older women. We know this because of the data developed from Hiroshima where young girls and women under the age of 20 who were exposed to radiation had a much higher risk of breast cancer when they reached middle age. But women who were already middle-aged when exposed to the radiation at Hiroshima did not show this increased risk.
Dr. Sam Epstein, Professor Emeritus Environmental and Occupational Medicine at the University of Illinois at Chicago, School of Public Health, says the dose is no trivial matter:
“Contrary to conventional assurances that radiation exposure from mammography is similar to that from a chest X-ray or spending one week in Denver, about 1/ 1,000 of a rad (radiation-absorbed dose) – the routine practice of taking four films for each breast results in some 1,000-fold greater exposure, 1 rad, focused on each breast rather than the entire chest. Thus, premenopausal women undergoing annual screening over a ten-year period are exposed to a total of about 10 rads for each breast. The premenopausal breast is highly sensitive to radiation, each rad of exposure increasing breast cancer risk by 1 percent, resulting in a cumulative 10 percent increased risk over ten years of premenopausal screening, usually from ages 40 to 50; risks are even greater for ‘baseline’ screening at younger ages, for which there is no evidence of any future relevance. Furthermore, breast cancer risks from mammography are up to fourfold higher for the 1 to 2 percent of women who are silent carriers of the A-T (ataxia-telangiectasia) gene and thus highly sensitive to the carcinogenic effects of radiation; by some estimates this accounts for up to 20 percent of all breast cancers annually in the United States.”[5]
Mammograms are a risk in more ways than one and finally, the discussion is going mainstream. But not without a fight.
Cancer is Big Business
| History of the Pink RibbonCharlotte Haley saw several women in her family battle breast cancer, so she handmade peach-colored loops in her dining room. Each set of five came with a card saying: “The National Cancer Institute annual budget is $1.8 billion, only 5 percent goes for cancer prevention. Help us wake up our legislators and America by wearing this ribbon.”… Then Self magazine and Estée Lauder wanted to use her ribbon. But Haley wanted nothing to do with it…Read more at Breast Cancer Action |
We do not have regular echocardiograms for heart disease, the number one killer in the United States.
Yet cancer-screening with the mammogram and the prostate specific antigen (PSA) blood test has captured more customers than all other efforts combined. More than $20 billion is spent annually on screening for these two diseases. Campaigns have been so effective that about 75 percent of men have had a routine PSA test and about 70 percent of women older than 40 report they have had a recent mammogram.[6]
The $20 billion spent each year for breast cancer and prostate cancer screenings represents a large vested interest. And that doesn’t include the income stream created by subsequent tests and medical interventions that come with an inconclusive or positive finding. Vested interests fight hard to maintain their turf.
The Task Force’s recommendations caused an uproar in large part because breast and prostate cancer screening have a problem that runs counter to everything people have been told about cancer: The screenings are finding cancers that do not need to be found because they would never spread and kill or even be noticed if left alone. That has led to a huge increase in cancer diagnoses because, without screening, those innocuous cancers would go undetected. Most cases of prostate cancer advance so slowly that a man will die of other causes before he would die of cancer.
Truth Be Told
Dr. Otis Brawley, chief medical officer of the American Cancer Society, told the New York Times in October: “We don’t want people to panic, but I’m admitting that American medicine has overpromised when it comes to screening. The advantages to screening have been exaggerated.” He took a lot of heat from even his own organization for saying that. Yet it was consistent with what he has been saying for decades. In 1997 he cautioned against PSA screenings:
“The benefits of screening and early detection, although theoretically possible, are yet unknown, whereas the risks and harms of screening and resultant treatment are definite. Although it [screening] may truly cure a few men who need to be cured, this benefit may be achieved at the cost of causing a large number of men with prostate carcinoma to undergo unnecessary treatment and resultant morbidity [illness].”[8]
PSA prostate cancer screening tests have not been shown to prevent prostate cancer deaths.
While the limits of cancer screening have long been known in the prevention community, the debate is new and confusing to many patients who have been told repeatedly to undergo annual mammograms and PSAs to detect cancer risk.
The ACS has long said that a mammogram is “one of the best things a woman can do to protect her health.” But the organization is said to be retooling its message in the wake of a study published in the October, 2009 Journal of the American Medical Association that analyzed breast and prostate cancer screening and questioned the legitimacy of such screenings in saving lives. The new ACS message will emphasize that screening for cancers can come with a real risk of overtreating many small cancers while missing cancers that are deadly.
“The health professions have played a role in oversimplifying and creating the stage for confusion,” said Dr. Barnett S. Kramer, associate director for disease prevention at the National Institutes of Health. “It’s important to be clear to the public about what we know and be honest about what we don’t know.”[9]
The Cancer Inside Us
We all have cancer cells inside us. As part of the normal daily process of metabolism, we all make somewhere between a few hundred to a few thousand cancerous cells. A healthy immune system recognizes these errant cells and takes them out before they get a chance to divide. Isolated cancer cells are not very strong.
There is universal agreement that cancer is a failure of the immune system. Cancer gets a foothold when your immune system is compromised.
The time it takes one cell to divide and become two cells is called the doubling time. The average doubling time is approximately 100 days[10,11]. Given that there are 365 days in a year, this means it typically takes about six years for the single cancer cell to become one million malignant cells, which together form a tiny tumor that is about the size of the tip of a lead pencil. A mass of this size is less than one millimeter in diameter, and is undetectable by breast self-exam, mammography, or by a PSA test.
Thus “early detection” with mammography or a PSA test is more of a marketing term than a reality. So too is the term “cancer survivor.” The way the cancer statistics are kept, a “cancer survivor” is a person who is alive five years after diagnosis. This does not necessarily mean a person who is cancer free.
Thermography – The Safe Option
Let’s see… Everyone admits radiation causes cancer… compression that takes place during a mammogram can spread cancerous cells… a cancerous mass is pretty far along by the time mammography can see it… So what if you could see the cancer forming years earlier without using radiation and compression?
This is the benefit of thermography.
As a tumor forms, it develops its own blood supply to feed its accelerated growth and this increased blood flow can increase the surface temperatures of the breast. Pre-cancerous tissues can start this process well in advance of the cells becoming malignant. Thermography measures the skin’s autonomic response to that inflammation – its “heat signature.” Modern thermography can detect suspicions of cancer’s formation sometimes 10 years earlier than mammography.
 |
 |
 |
| Baseline | 3 Months | 6 Months |
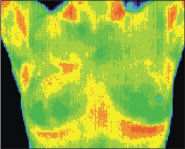
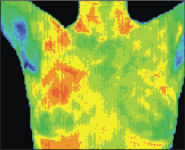
The pictures show the development of breast cancer in the right breast. The cancerous tissue appears red because of the heat generated by the greater metabolic activity and the increased blood supply of the cancerous tissue.
At the Arizona Center for Advanced Medicine, we use thermography to look for early, tell-tale signs of a possible malignancy. We look for asymmetry in the heat pattern due to temperature differences between the two breasts. Does there seem to be a “hot spot” in one breast that grows larger over time? A series of thermograms over time gives us the ability to observe any asymmetry.
Thermography can spot suspicious tissue 10 years before it can be detected by mammography.
Mammograms look at structure; they detect a cancerous mass. Thermograms look at systems; they can detect early suspicions of cancer formation. Thus thermography is clearly the better early warning system.
| Thermography | Mammography |
|
• A functional test which detects the body’s cutaneous sympathetic
response to underlying inflammation.• Inflammation is detectable
by thermography almost immediately• Early detection is best prevention•
No ionizing radiation• No compression (squeezing)
• No problem with fibrous and dense breasts, or implants |
• An anatomic test which detects calcification and/or fairly large
masses• Does not detect early inflammatory change which eventually
results in cancer• Tumor is detectable generally after it has been
in the body for 10 years• Ionizing radiation• Compression (squeezing)
• Problem with fibrous and dense breasts, and with implants |
The Politics of Medicine
Thermography has a lot going for it. Except it is on the wrong side of the political divide.
When you are referred for a mammogram or PSA test, the doctor is likely following the guidelines of the two leading national cancer research and information organizations primarily responsible for setting public health policy on cancer screening: The American Cancer Society (ACS) and the National Cancer Institute (NCI). Both, along with other well-funded, high-profile organizations, such as Susan G. Komen for the Cure (SGK), recommend regular mammogram screening of symptom-free women beginning at age 40 – and they say they will maintain that position despite the new Task Force guidelines.
Both ACS and SGK have connections with numerous corporations in the chemical, cosmetic, and pharmaceutical industries, many of which derive substantial income from the screening and treatment of breast cancer. There is more money in the detection and treatment of breast cancer than in preventing it, and that leads to an enormous conflict of interest.
SGK for example owns stock in General Electric, one of the largest makers of mammogram machines in the world. Radiologists sit on the on the SGK board. Get the picture?
Many people invested early on in mammography. Thermography was viewed as a competitor. Lobbying efforts some years ago at the American Medical Association’s House of Delegates and at Medicare brought about the removal of thermography coverage by insurance companies. To this day, the American Cancer Society still promotes only mammography, despite its dangers.
Recent advances in technology have brought thermography to the point where it is now used as one of the diagnostic tools in two cancer research centers in North America. Today, there are very strict protocols both for testing and interpreting. Perhaps due to these guidelines, thermography (unlike digital mammography) has exploded in its technique and capabilities.
It’s the Environment, Not Genetics
Many breast cancer advocates disagree with the way the public is told to think of breast cancer – take your annual mammogram, don a pink ribbon, run to raise money for research, and celebrate the survivors. Problem is, these approaches are not making much of a dent.
The American Institute for Cancer Research and the World Cancer Research Fund analyzed 1,000 studies – the largest review ever of the research examining lifestyle and breast cancer – and determined that lifestyle is a strong modifiable risk factor for breast cancer breast cancer. “It is now very clear that lifestyle is a strong modifiable risk factor for breast cancer, but I don’t think women have really gotten the message,” said epidemiology professor Elisa Bandera, MD, PhD, who helped write the 2009 report. “Women tend to overestimate the role of genetics in breast cancer and underestimate lifestyle.”
| “The cosmetics industry has borrowed a page from the playbook of the tobacco industry, by putting profits ahead of public health. Cosmetics can be dangerous to your health. Every woman who uses face cream, or hair spray, or lipstick, or shampoo, or mascara, or powder should demand that this arrogant and irresponsible power-play by the industry be rejected. A study by the respected, non-partisan General Accounting office reported that more than 125 ingredients available for use in cosmetics are suspected of causing cancer.”– Senator Ted Kennedy, September 1997, during debate of a bill to reform the FDA– As reported by Phillip Day, Cancer, Why We’re Still Dying to Know the Truth, 1999, p 92 |
The study concluded that 40% of all cancers could be prevented with “simple” lifestyle changes such as maintaining a healthy weight, eating well, exercising, and limiting alcohol consumption.[12]
Two years earlier, a review spearheaded by the Silent Spring Institute also concluded that the environment fuels cancer. “Laboratory research provides evidence that environmental pollutants may contribute to breast cancer risk by damaging DNA, promoting tumor growth or increasing susceptibility by altering mammary gland development … These compounds are widely detected in human tissues and in environments, such as homes, where women spend time.”
The review found that the relative risks associated with PAHs (largely from car exhaust) and PCBs were “comparable in magnitude” to many breast cancer risk factors that have received more attention, such as age at first full–term pregnancy and inactivity.
The majority of cancers are caused by changes in the cellular DNA because of damage due to the environment. Environmental factors responsible for causing the initial mutation in the DNA are carcinogens, and there are many of them in our daily environment. This is the science of epigenetics, the fact that stress, diet, behavior, toxins and other factors activate chemical switches that regulate gene expression. In other words – the way your genes express themselves changes in response to changes in the environment and this can determine whether or not you get cancer.
A tiny fraction of cancers can be blamed on one’s inherited genetics. Less than 5% of all cancers are thought to be purely hereditary.[13]
Silent Spring’s Julia Brody noted that the media doesn’t do much with press releases about studies showing breast cancer to be an environmental disease. “We need to act on the weight of the evidence as it evolves. We waited too long on tobacco smoke, we waited too long on lead.”
Still Waiting for Prevention Campaigns
To date, none of the big players has launched major education campaign. The commonly stated preventive recommendations typically look like this:
• Be physically active.
• Maintain a healthy weight. (The average American no longer has
a healthy weight.)
• Cut down on “bad” fats and eat more “good”
fats like olive and canola oil. (No warning to avoid genetically modified
foods – some 80% of the canola grown in the U.S. and Canada is now
GM, according to Jeffrey Smith, Executive Director of the Institute for
Responsible Technology)
• Take a daily multivitamin with folic acid. (No discussion of the
absorbability of different forms of vitamins.)
• Limit alcohol.
• If possible, choose to breastfeed children.[14]
The ACS website does provide a long list of possible and known carcinogens including benzene, HRT, formaldehyde, petroleum products, coal tar shampoos, aluminum, mineral oil, Aflatoxins, arsenic, etc.[15] However, the list is not user friendly or informative. For example, it does not tell you that you are likely to encounter arsenic in every package of non–organic chicken. Or that Aflatoxin can contaminate virtually any grain, fruit or vegetable that has been stored in conditions permitting the growth of mold and that peanuts seem to be especially vulnerable.
The NCI does a better job of it. They have a downloadable booklet entitled, Cancer and the Environment, that is easy to read:
|
Polycyclic aromatic hydrocarbons (PAHs)
A number of studies show increased incidence of cancer (lung, skin and urinary cancers) in humans exposed to mixtures of polycyclic aromatic hydrocarbons (PAHs). The primary source of PAHs is from burning carbon-containing compounds. PAHs in air are produced by burning wood and fuel for homes. They are also contained in gasoline and diesel exhaust, soot, coke, cigar and cigarette smoke and charcoal-broiled foods. In addition, they are the byproducts of open fires, waste incinerators, coal gasification, and coke oven emissions. Foods that contain small amounts of PAHs include smoked, barbecued or charcoal-broiled foods, roasted coffees, and sausages. |
No Money in Prevention?
Who is going to pay to publicize the proven benefits of vitamins D and C, of desiccated thyroid and iodine, of omega 3s and grass-fed beef? These work horses of prevention have no “heavy hitter” corporate sponsors.
Foundations and even government agencies get funding from corporate entities with deep pockets – that’s just how the world works. Sometimes those lucrative sponsorships come from companies that add to the carcinogens to our environment and make unhealthy foods.
Let’s look at one such sponsorship. For those with cancer, sugar is definitely on the Do Not Eat list. The Nobel prize-winning biochemist and medical doctor Otto Warburg discerned by 1930 that cancer cells use more sugar than healthy cells, hence the modern phrase, “sugar feeds cancer.” In fact, when you undergo a PET scan looking for tumors, the radioactive agent is combined with sugar water because cancer cells take up the sugar so much faster than healthy cells.
One of SGK’s regular corporate sponsors is M&M candies:
“From August 15 through October 31 [2009], Mars will once again sell specially marked bags of dark pink and light pink M&M’S® Brand chocolate candies in grocery and retail outlets throughout the nation. In conjunction with this program, they will make a guaranteed donation of $500,000 to Komen for the Cure.”[16]
Over the years, criticism has been heaped on the NCI, the ACS, SGK, and others for the conflicts of interest generated by board members and sponsorships. Dr. Samuel Epstein of the Cancer Prevention Coalition, and Ralph Moss, PhD, have been particularly vocal about conflicts of interest, and the focus on money-generating screenings and treatments rather than prevention. The group Breast Cancer Action launched the “Think Before You Pink” campaign to draw attention to the fact no one seems to know where the money raised for research goes, and if the research is even asking the right questions.
Learning About Prevention
Two groups who are out front about prevention of breast cancer publish State of the Evidence: The Connection Between Breast Cancer and the Environment, a succinct resource for the environmental toxins linked to breast cancer. First released in 2002 and updated in 2003, 2004, 2006 and 2008 to include new research findings, the latest report synthesizes the results of more than 400 studies, runs 147 pages long with 667 references, and was vetted by five independent experts. It is published by the Breast Cancer Fund, a national nonprofit focused on environmental and other preventable causes of the disease, and Breast Cancer Action, a membership organization that “challenges assumptions and inspires change to end the breast cancer epidemic.”
The 2008 edition explains that the latest data “show that we need to begin to think of breast cancer causation as a … web of often interconnected factors, each exerting direct and interactive effects on cellular processes on mammary tissue,” and points to growing evidence that “exposure of fetuses, young children and adolescents to radiation and environmental chemicals [notably the pesticide DDT] puts them at considerably higher risk for breast cancer in later life.” Though disturbing, the report’s underlying message is hopeful: “By decreasing exposures to carcinogens … we may continue to lower breast cancer level – and actually prevent the devastating disease – in the future.”
We know that our body’s innate wisdom stores environmental toxins in fat – safer than storing it in organs. Not surprisingly, obesity is now widely recognized as the most important modifiable risk factor for breast cancer among postmenopausal women. About three out of four breast cancers in this age group are fueled by the hormone estrogen, which is also produced in fat tissue. Estrogen levels in overweight, postmenopausal women are 50% to 100% higher than among lean women, according to the National Cancer Institute.
Breast cancers also tend to be detected later in overweight women, mainly because tumors are harder to detect with mammography.
Learning how to detoxify as a part of losing weight is a big – but often unspoken – piece of the puzzle. That is why at the Arizona Center for Advanced Medicine, we developed a weight loss program that incorporates detoxification, and we monitor your progress to minimize cleansing reactions.
Cancer is Preventable
An unfortunate aspect of annual screenings is that they create a passive state, an annual period of waiting to find out if cancer has claimed you, as if there is no way you can exert control over your own life.
It is much easier to prevent cancer than to reverse it. It takes curiosity, knowledge, and a willingness to change some everyday routines. Click on the “P” to the right and access our easy tutorial on what to do for preventing cancer.
The U.S. Task Force made a good call in recommending against regular mammograms for women aged 40-49. If in all the controversy, more focus falls on prevention, then the Task Force will have accomplished a great deal of good for women.
It is time to talk more openly about preventing cancer.
[1] Saving Women’s Lives: Strategies for Improving Breast Cancer Detection and Diagnosis. National Academy of Sciences 2005 publication.[2] http://www.cancer.gov/cancertopics/understandingcancer/genetesting/Slide27[3] John W. Gofman, M.D., Ph.D., Radiation from Medical Procedures in the Pathogenesis of Cancer and Ischemic Heart Disease, C.N.R. Book Division, Committee for Nuclear Responsibility, Inc., San Francisco, 1999[4] Julie Steenhuysen, Mammogram Radiation May Put Some Women at Risk, ABC News, December 1, 2009. Accessed at http://abcnews.go.com/Health/wireStory?id=9218026[5] http://www.preventcancer.com/patients/mammography/dangers.htm[6] L Esserman, Y Shieh, I Thompson; Rethinking screening for breast cancer and prostate cancer, JAMA. 2009 Oct 21;302(15):1685-92.[7] Gina Kolata, Cancer Group Has Concerns on Screening, New York Times, October 31, 2009. Link[8] Otis Brawley, Prostate carcinoma incidence and patient mortality. The Effects of Screening and Early Detection. Cancer, 80:1857-1863, 1997[9] Tara Parker-Pope, Benefits and Risks of Cancer Screening Are Not Always Clear, Experts Say; New York Times, October 21, 2009. Accessed at http://www.nytimes.com/2009/10/22/health/22screen.html?_r=1[10] P Gullino; Natural history of breast cancer. Progression from hyperplasia to neoplasia as predicted by angiogenesis. Cancer. 1977 Jun;39(6 Suppl):2697-703.[11] S Friberg, S Mattson; On the growth rates of human malignant tumors: implications for medical decision making. J Surg Oncol. 1997 Aug;65(4):284-97.[12] Salynn Boyles, Lifestyle Changes Cut Breast Cancer Risk – Researchers Say Exercise and Diet May Prevent Some Cases of Breast Cancer, WebMD Health News, Sept. 3, 2009. Accessed at http://www.webmd.com/breast-cancer/news/20090903/lifestyle-changes-cut-breast-cancer-risk[13] National Cancer Institute’s publication, Cancer and the Environment, page 2[14] http://ww5.komen.org/BreastCancer/HealthyBehaviorsampRisk.html[15] http://www.cancer.org/docroot/PED/content/PED_1_3x_Known_and_Probable_Carcinogens.asp?sitearea=PED[16] http://ww5.komen.org/ContentSimpleLeft.aspx?id=14366
