Colorectal Cancer:
Colon cancer is cancer of the large intestine. Rectal cancer is cancer of the last several inches of the colon. Together, they are often referred to as colorectal cancers.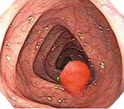
Most cases of colon cancer begin as a small, benign (not cancerous) polyp or lesion. Sometimes these growths later become cancerous.
Colon cancer is the third most commonly diagnosed cancer for both men and women - after breast and prostate.
If you have an inflamed gut, your odds of coming down with colon cancer go way up. People who have ulcerative colitis, for example, are more apt to develop cancer of the colon or rectum.[1]
If you have a history of colorectal cancer in your family, you may be predisposed to elevated levels of COX-2 enzymes. These cause inflammation in the gut. Angiogenesis, the blood vessel development essential to tumor growth, requires COX-2 enzymes. Over-expression of COX-2 leads to increased expression of VEGF, vascular endothelial growth factors, the messengers that ask for more blood vessels to be made.[2,3]
When colorectal cancer runs in families, it tends to show up about age 39, instead of after age 55. Polyps may occur in the preteen and teen years, and tumors tend to grow more rapidly.[4]
People with higher levels of IGF-1 receptors have an increased risk of developing colorectal cancer.[5,6] Insulin can bind to two different receptors: insulin and IGF-1 (insulin-like growth factor-1) receptors. When insulin binds with an insulin receptor, blood sugar levels go down. But when insulin binds to IGF-1 receptor, it mainly induces cell proliferation. Most tumor cells are dependent on the IGF-1 receptor signal pathway for their development.
Composition of the bacterial flora of the GI tract is also believed to play a role in the development of both inflammatory bowel disease and cancer.[7] The gut harbors a virtual army of bacteria to digest food and make vitamins. The greatest numbers of bacteria in the colon are the Bacteroides, a group of Gram-negative, anaerobic, non-spore forming bacteria. They have been implicated in the initiation of colitis and colon cancer. In a healthy body, they are held in check by the Bifidobacteria, the Gram-positive, non-spore forming, lactic acid bacteria often described as the “friendly” bacteria. Composition of the flora is influenced by breast feeding (human milk contains stimulates the growth of Bifidobacteria), cultural conditions, age, diet, and the use of antibiotics.[8]
Overweight people are more likely to get colon cancer. A 2010 study found that obese men are 35 percent more likely to die of colon cancer over the next eight years than men of normal weight. Obese women are 25 percent more likely to die of the condition than women of normal weight.[9] Gaining weight causes your hormones to get out of whack - and those imbalances can fuel colon cancer and other diseases.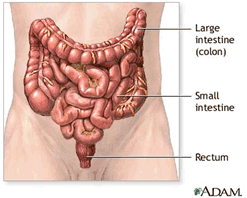
What is the colon, and what purpose does it serve?
The colon is one of the first organs to develop, after the brain. It is about 60 inches long. We call it the large intestine, the last part of the digestive system.
The colon's basic job is to separate solids from liquids, reabsorb the liquids and eliminate the solids - that which no longer serves the body.
Ideally, food that enters your body should pass all the way through within 36 hours - that's called transit time. If transit time is too slow, gas, putrefaction, and fermentation can set in.
When things are not working right because of slow transit time or bacterial imbalance, bile acids - upon reaching the colon - can be converted into carcinogenic substances. Staying in contact with the colon walls for long periods of time, these substances can possibly be a cause of colon cancer. Toxins, poisons, and free radicals from the plaque itself and from pathogenic bacteria and parasites living in and under the plaque constantly seep into the bloodstream and lymph, settling in the weaker areas of the body, especially the liver, kidneys and spleen. Bile acid breakdown products (lithocholates) also signals the liver to decrease bile acid production.
 The intestinal tract has layers of smooth muscle, both circular and longitudinal, which serve to propel food and waste toward their final destination. Between the two layers ride the autonomic nerves which manage both our digestion and our excretion functions without us having to pay attention to these functions. We consciously control the striated muscle in the mouth, the upper part of the esophagus, and in the lower part of rectum and anus.
The intestinal tract has layers of smooth muscle, both circular and longitudinal, which serve to propel food and waste toward their final destination. Between the two layers ride the autonomic nerves which manage both our digestion and our excretion functions without us having to pay attention to these functions. We consciously control the striated muscle in the mouth, the upper part of the esophagus, and in the lower part of rectum and anus.
The gut also has a role that is hard to describe in the medical books. "He had a gut feeling about that," or, "What does your gut tell you?" We hear these things all the time. Many of our emotions are seated in the gut where the majority of our serotonin is made.
In a very real sense, constipation reflects the ability to hold onto the past, or the inability to let go of the past. One of the extraordinary things about the intestinal tract is that whereas much of it is NOT under voluntary control (small intestine, right side of colon), we actually do have voluntary control of both ends - the mouth and the anus. We can choose what goes in, and we can choose what comes out. We can hold on to things if we so decide. The holding on may be on a conscious or subconscious level, but it is ultimately under our conscious control. The nerves in those areas have both autonomic and voluntary connections with different kinds of muscle - both smooth and striated.
We are energetic and spiritual beings with physical bodies. What happens on one level happens on all levels. There is a wonderful treatment in Chinese medicine called "External and Internal Dragons," which is aimed at restoring physical, emotional, mental and spiritual balance to the body. One of the points used is the colon - to eliminate on all levels those things which no longer serve a useful function, which are holding us back physically and emotionally.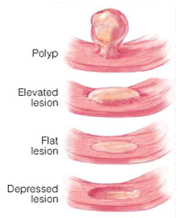
What are polyps and flat lesions?
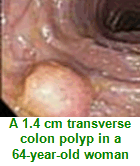
Colorectal polyps are growths projecting from the colonic or rectal lining. They are extremely common. Their incidence increases as individuals get older. Half of all people over the age of 60 harbor at least one polyp. Polyps greater than one centimeter have a greater cancer risk associated with them than polyps under one centimeter; risk factors include advancing age or a family history of colon cancer or polyps. The outlook for patients with colorectal polyps is excellent when the polyps are removed. Polyps that are left behind can develop into cancer over time.
Flat lesions are like moles of the colon. They are harder to see on CT scans and colonoscopies. Flat lesions tend to be more dangerous because they are more likely to be cancerous than a protruding polyp. They are also more common in the U.S. population than previously thought. A study of 1,819 veterans who underwent elective colonoscopy in California was published in 2008 in The Journal of the American Medical Association.[10,11] The study found flat lesions in roughly 9% of patients who underwent colonoscopy. Also, flat lesions were roughly five times more likely to contain cancerous tissue than polyps, after adjusting for polyp size.
Testing and Diagnosis
Colonoscopies - the test where they use a tiny camera on the end of a long tube inserted into the rectum to look at it and the large intestine - is among the best of the cancer screening tests. Mammogram and prostate screening tests have gotten a deservedly bad rap for not being particularly good at finding cancer, and mammograms use cancer-causing radiation. Colonoscopies pose no harm to the body except for the "clean out" products so many doctors use before the test. The FDA even required some of the preparations to have black box warnings. At the very least, these products can be extremely irritating. One of my patients who underwent a traditional clean-out procedure prior to a colonoscopy was told he might have irritable bowel, but it might also be just irritation from the clean-out products. The doctors couldn't tell so they wanted him to repeat the test. He decided that made no sense. The prep for a colonoscopy can now be done safely, and we think more comfortably, with a simple colon hydrotherapy session.
A Canadian study, published December 2008 in the medical journal Annals of Internal Medicine, found that colonoscopies are less accurate than expected. This study found that the test missed just about every cancer in the right side of the colon. That is where about 40 percent of the cancers arise, but are harder to detect. (Flat and depressed lesions tend to cluster in the right colon.) This study also found the test missed roughly a third of cancers in the left side of the colon. So instead of preventing 90 percent of cancers, as previously thought, colonoscopies prevent perhaps 60 percent to 70 percent. But contrast that with PSA tests that have not been shown to prevent prostate cancer deaths at all.[12,13] And colonoscopies can remove non-cancerous polyps.
Colorectal cancer may be suspected if you see blood in the stool, or if an occult blood test is positive. Many conditions may manifest blood in the stool, including hemorrhoids, infectious diarrhea, Crohn's disease, ulcerative colitis, and other inflammatory bowel conditions. Rectal examination may show evidence of a mass if we are dealing with a cancer low in the colon. CT scan or MRI may show X-ray evidence of a mass and usually must be followed by a colonoscopy to retrieve tissue.
None of the tests themselves gives a definitive diagnosis. Only examination of tissue under a microscope provides the diagnosis. Many efforts have been made to diagnose a cancer without having to get a piece of the tumor surgically. Tumor markers are proteins which are sometimes found in high amounts in the bloodstream. Until we see microscopic evidence of abnormal tissue, we only have a suspicion. Tissue is the gold standard.
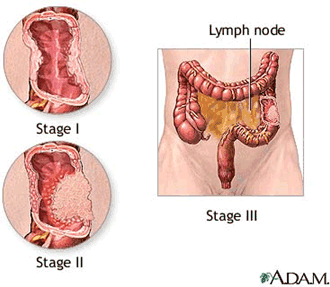
Patients are given an estimate of prognosis, an estimate of the cancer's severity based on what stage it is in - how far along it is. Staging is based on tumor size in centimeters (T), number of positive lymph nodes (N) and the presence or absence of metastases (M) - this is called TNM staging, with stage one being T0, N0, M0 and stage IV being any size T, any number of N, and presence of metastases.
| Stage grouping | 5 year survival | |
| 0 | Tis, N0, M0 | |
| I | T1 or T2, N0 M0 | 74% |
| IIA | T3, N0, M0 | 67% |
| IIB | T4, N0, M0 | 59% |
| IIIA | T1 or T2, N1, M0 | 73% |
| IIIB | T3 or T4, N1, M0 | 46% |
| IIIC | Any T, N2, M0 | 28% |
| IV | Any T, any N, M1 | 6% |
Conventional Treatment
Standard allopathic treatment of colorectal cancer is usually surgical, if the tumor in fact can be removed surgically. When polyps turn cancerous, you take out more then just the polyp. You take out about half the colon to account for lymphatic drainage and then resect it - connect the remaining ends of the colon together. The intestinal lining replaces itself quickly and that helps healing.
In recent years, these tumors have been removed laparoscopically, with good results and fewer side effects after surgery, less time spent in hospital, and faster resumption of normal bowel function.[14]
Statistics tell us survival after surgical resection is about 50-60% at 5 years after treatment.[15]
Unfortunately, there is widespread micrometastasis which occurs early in the course of any given cancer, so the potential for recurrence of cancer is almost always high. Tumors shed cells into the bloodstream. Micrometastasis is when small clumps of tumor cells settle into tissues and start to get a foothold. The body deals with the situation as best it can - a strong immune system can knock them out these clumps; a weak immune system does not. Also, if years later, the person undergoes some manner of major stress, the immune system may lose its ability to stay on top of things and the cancer may return.
A silver bullet type drug to stop tumors is always being tried, but success is elusive. The experimental drug PLX4032, which promises to reverse the effects of a gene variant that affects both melanoma and colon cancers, is a good example. It produced seemingly good results in some patients with melanoma, but failed miserably for patients with colorectal cancer. Same drug, same gene mutation, different result. "We've gone through a very rapid period of high expectations, maturation and disappointments," Dr. J. Leonard Lichtenfeld, the deputy chief medical officer of the American Cancer Society, told the New York Times in 2010. "I think there was almost a naïveté that if we could find the target, we would have the cure."[17]
Chemotherapy does stop tumors. It is generally recommended when there is evidence the cancer has returned, unless it clearly has spread into the lymph nodes - stage 3 or 4. The conventional stats tell us that with chemotherapy, these patients may live another two to three years. This is a particularly negative prognosis which reflects the debilitating nature of conventional, full-dose chemotherapy. In these cases, the person's health is already compromised and full dose chemotherapy further degrades the immune system and health of the organs.
 Many chemotherapy regimens have been studied. The most commonly used are FOLFOX (leucovorin, 5-FU and oxiplatin) and FOLFIRI (leucovorin, 5-FU and irinotecan).
Many chemotherapy regimens have been studied. The most commonly used are FOLFOX (leucovorin, 5-FU and oxiplatin) and FOLFIRI (leucovorin, 5-FU and irinotecan).
Addition of monoclonal antibodies statistically increase survival a median of about 2 years in those patients with metastatic disease at the time of diagnosis, in those patients with the right genetics.[18] The use of monoclonal antibodies involves injecting immune system antibodies like lymphocytes - giving you antibodies that your immune system should generate but does not. However, these injected antibodies don't always act as they should - the can inadvertently trigger a hyperactive immune response.
The grim survival statistics would likely be much improved if traditional oncology would:
• Declare the one-size-fits-all approach (sometimes called "cookbook medicine") obsolete and do chemo-sensitivity testing for each individual patient to determine which drugs are going to do the best job of killing cancer cells, given the particular genetic profile of that person's cancer cells.
• Use low-dose chemotherapy, potentiated (made more powerful) by the use of insulin to target the drugs to the cancer cells, by-passing healthy cells.
• Take time to nourish the body with nutrients, rebuild the immune system, and teach patients that cancer is an environmental disease - very much a product of diet and environment - and there are things we can all do to make our bodies less hospitable to the growth of cancer clusters.
In 1991, Dr. Albert Braverman, Professor of Hematology and Oncology at the State University of New York, Brooklyn, published an article in the British medical journal Lancet titled “Medical Oncology in the 1990s,” in which he wrote:
“The time has come to cut back on the clinical investigation of new chemotherapeutic regimens for cancer and to cast a critical eye on the way chemotherapeutic treatment is now being administered.”[19]
The calls for change began decades ago, but implementation is painfully slow.
Is there a way to tell if chemotherapy will be successful? Is the pain worth the gain?
Maybe not, unless you do the three things bulleted above. It's up to you.
Micrometastases are all genetically different. When tumors shed cells into the blood stream, the tumor cells have different DNA. By definition, tumor cells are genetically wild and they don't all mutate in the same direction. We can greatly increase the odds of stopping cancer when a chemo-sensitivity test can tell us which drugs will work best against those genetic profiles.
Once you identify the most effective chemotherapy regimen to use, then the issue is delivering it to the cancer cells without also endangering all the non-cancerous cells. New advances in chemotherapy have found out how to do that.
Conventional chemotherapy attacks all rapidly dividing cells, cancerous and healthy, which is why standard chemotherapy has such severe side effects such as decreased white blood cell count, hair loss, mouth ulcers, diarrhea, and organ failure.
But when we look at what makes cancer cells different than non-cancerous cells, we see a couple of key differences that make cancer cells vulnerable. Whereas healthy cells can use fat for fuel, cancer cells must use glucose (sugar) for fuel. To make it easy to get a lot of glucose from the bloodstream, cancer cells cover themselves with insulin and insulin-like growth factor receptors. Insulin opens the cell wall and escorts the glucose inside the cell. Donato Perez Garcia, MD, discovered in the early 1930s that giving insulin to a patient would allow more antibiotic drugs to penetrate the blood brain barrier. In subsequent years he discovered that the same technique would allow more chemotherapeutic drug to enter cancer cells, thus opening the way for targeted chemotherapeutic treatments that do not bombard the healthy cells. This treatment is called "Insulin Potentiation Therapy, or IPT for short. Click here to read more about IPT.
Tell me more about the genetics of a tumor.
We use a simple blood test (not available in this country) to look for circulating tumor cells (CTCs) in the blood.[20] We know that tumors have a very high potential for metastasizing (spreading) by shedding tumor cells into the circulating blood. CTCs will not always give us a good indication as to their source. In other words, you could find CTCs but possibly we cannot tell if they come from the colon cancer we know you have or the small pancreatic cancer we don't yet even suspect.
We tend to think about "cancer" as a single disease, and "colon cancer" as a place where the disease happened to hit, that all colon cancer cells are exactly the same, and have the same altered genetics which allowed them to escape from the immune system's control in the first place. However, it is quite clear from the literature that not all tumors are created equal, and not all cells originating in the same tumor have the same genetic expression.[21,22]
You may have heard that the gene variants BRCA1 and BRCA2 can predispose a person to breast cancer. When looking at cancers associated with the gastro-intestinal tract, we look for the K-Ras and p53 gene variants because they are associated with GI cancers in a high proportion of patients.[23]
Balance is important in nature, and that is especially true for a key part of the cancer equation where cell growth goes out of control.
Our bodies make EGF - epidermal growth factor. This is what makes skin cells grow. Too little and you have sclerodema, hardening of the skin. Too much and you feed the growth of tumor cells. The tumor secretes EGF receptors which activate the K-Ras gene asking it to send out growth factors so the cells divide more so the tumor grows more.[24]
Drugs have been developed to target the receptors for EGF molecules and restrain them from contributing to the growth of tumors. The drugs cetuximab and panitumumab have been shown to increase disease-free survival, when given in combination with standard chemotherapy protocols, particularly FOLFIRI AND FOLFOX, depending upon the individual person's genetics.
Yale alumni M. Wasif Saif, MD, and Manasi Shah, MD, studied the data on how well those drugs work. They found that patients with mutant K-Ras did not benefit, but patients with wild-type K-Ras benefited significantly. Drs. Saif and Shah recommend that oncologists ascertain the K-Ras status prior to initiating treatment with these drugs (monoclonal antibodies). They conclude:
"We are entering an era of personalized medicine in cancer therapy where treatment is tailored to the individual. The predictive value of K-Ras mutations in the treatment of mCRC [metastatic Colorectal Cancer] is very useful to clinicians and patients in terms of decision making, avoiding toxicities, and decreasing financial burden."[25]
How do we lessen the odds my colon cancer will come back?
First rule of thumb in medicine: Do No Harm. The treatment cannot be so harsh that although you've killed the tumor, you've left the body too weak to resist the daily assaults to the immune system in the months and years ahead. A healthy immune system is the best insurance against cancer and other chronic diseases. In our opinion, the toxicity of full dose chemotherapy significantly lessens the odds of survival, and combining low-dose targeted chemotherapy with other less toxic ways to kill cancer cells, while nourishing other parts of the body, significantly increases the odds of survival.
Many complementary therapies have been used around the world for treatment of cancer over the millennia, not just chemotherapy drugs. Therapeutic doses of vitamin C, given intravenously, kill cancer cells.[26] Some botanicals are powerful, such as Iscador®, for example. It is made from the fermented extracts of the mistletoe plant. Iscador has been shown to kill cancer cells in the laboratory.[27] A 30-year-long study with more than 35,000 participants found that Iscador greatly improves survival rate for a wide variety of cancers. Study participants who augmented conventional therapy with mistletoe extract survived 40% longer compared with those who didn't use the plant therapy.[28] Unfortunately this botanical is no longer available in the United States, since the Federal Drug Administration has banned its importation.
A 2009 study found that higher blood levels of vitamin D may double survival rates of colorectal cancer patients. People with the highest average levels of 25-hydroxyvitamin D had a cancer-specific mortality half that of people with the lowest average levels. What's more, high levels of the vitamin were associated with an overall mortality level 40 percent lower than people with the lowest average levels.[29]
In treating your cancer, we want to both kill the cancer and nurture your immune system so it can defend against the return of cancer.
CASE STUDY:Although "Carole" had experienced GI issues for years, she had been doing a gluten-free diet, and feeling fine. But one morning she passed out at the breakfast table. I did a blood test. The overall results were not bad for a woman in her early nineties, with one notable exception - she had a very low hemoglobin count, 7.8, so she was losing blood somewhere. A stool test was positive for blood, but not so much so that Carole would have seen it. I scheduled a CT scan, which showed a mass on the right side of the colon - with suggestion of swelling in the local lymph nodes - at least a stage 3 disease. The gastroenterologist ordered blood tests for tumor markers. They were all negative. Her tumor was not producing the proteins, the markers, they were looking for. We had an AMAS test which confirmed anti-malignin antibodies; it picked up on the immune system's response to the tumor. We still did not have an absolute diagnosis of cancer.
Surgery was scheduled. The surgeon performed both a colonoscopy to confirm the presence of a tumor, and the subsequent surgery to remove half her colon. The laparoscopic colectomy was very elegant and saved her body a lot of trauma. Carole was out of the hospital in five days; that's unheard of for someone of her age. I sent off a piece of the tumor to Germany for the BioFocus test so we would know what drugs and complementary therapies would be most effective.
As I write this, Carole has finished her twelfth IPT treatment, and we just did a blood test. She has a white blood cell count (WBC) of 4.2 and an absolute neutrophil count (the white cells that knock out infection) of 2.8. Both values are well within normal limits. Her initial WBC was 7.6 with 5.7 absolute neutrophils count, so she really did not lose much ground with the treatments.
This tells me the IPT has spared her immune system. After conventional chemo, within about 2 weeks you typically see a WBC of 1.0 or less. The white blood cells tend to get killed en masse by the bombardment of so much chemo; conventional chemo sessions are scheduled about 3-6 weeks apart because it kills so many neutrophils and they must regenerate before the chemo can be administered again; infection is a large and growing problem in conventional chemotherapy.
Carole has experienced no nausea, vomiting, hair loss, heart arrhythmias, ulcerations of the mucus membranes - all standard side effects of the chemotherapy drug Fluorouracil. She called me the day after her first treatment and said, "Martha, I feel wonderful." She often takes a nap after her treatments, but she is always up and about the next day - and she is in her 90s!
How to prevent colorectal cancer
About one in three people die of their disease every year because they didn't catch it soon enough or because it was very aggressive. Current guidelines call for colonoscopy screenings to begin at age 50. However, if you have a family history of colorectal cancer, consider starting screening at age 35. If treated, you have a 90 percent chance of being alive in 5 years.
The National Cancer Institute's website states:"Colorectal cancer prevention is a clinical imperative, and a key part of prevention involves the search for drugs that can safely and effectively block or reverse colorectal cancer development."
We certainly agree with the prevention part of the statement. However, it is important to realize that prevention begins LONG before drugs are necessary. As we've seen from the headlines in recent years, drugs too often come with nasty side effects.
Anti-inflammatory drugs are known to reduce the incidence of GI cancers.[30] However, these Cox-2 inhibitors are also associated with increased cardiovascular risk, so it would appear that drug therapy is not good prevention.
The best way to prevent colon cancer is to prevent chronic inflammation which hides unseen and unfelt in the body. Only when its symptoms raise their ugly head, be it through cancer, heart disease, diabetes, or some other chronic illness, do we know this sneaky culprit has been sapping our health.
Adherence to the Mediterranean diet may be the best preventive measure we could possibly take.[31,32] This nutritional program emphasizes olive oil, nuts, fish, fresh fruits and vegetables, and whole grains. High fat meats, processed foods, and vegetable oils are very limited. Bottom line: good food has cancer protective agents. When cancer has actually developed, then we need to be even more strict about eliminating carbohydrates in the diet.
Sugars and starches tend to be highly inflammatory foods, and should be eaten only occasionally, if we wish to avoid inflammation in the gut. Foods to which the individual is allergic or sensitive also are inflammatory. Fruits and vegetables contain nutrients which our bodies need, and are seldom inflammatory. Red meats are considered "hot" in Chinese medicine, and are more inflammatory than poultry or fish. Western literature demonstrates that commercially raised meat and fowl have acidic bodies because they have been fed an unnatural diet of grains, corn, and soy. When we in turn eat meat from such animals, our bodies become more acidic than if we had eaten grass-fed beef or pasture-raised chicken or non-farm raised fish. When naturally alkaline vegetables are eaten with naturally raised meat and dairy products, the veggies balance the acidity in the meat and dairy. Commercially raised animals are also given steroids, hormones, antibiotics, and sometimes arsenic which are unhealthy for us to consume.
Probiotics will help to restore the normal gut flora which antibiotics have often destroyed. In addition, they reduce inflammation in the gut, and sometimes even help to potentiate certain forms of chemotherapy.[33] Our ancestors got their daily doses of probiotics from raw and fermented foods. We don't consume much of either today. Supplements are a good alternative, just make sure they have been formulated to survive the stomach acid.
Vitamin D plays a big role in cancer prevention. Many studies have found that men with higher amounts of vitamin D significantly reduce their risk of developing colon cancer.[34] A study dating back to 1989 followed more than 25,000 people for eight years and discovered that people with vitamin D levels of 33-41 ng/ml, which is still a fairly low vitamin D level, reduced their risk of colon cancer by 80 percent.[35]
Prevention starts with what goes in to the gut ... prevention can be initiated at any time. Just because you already have colon cancer does not mean it's too late. Today can be indeed the first day of the rest of your life.
[1] A Ekbom, C Helmick. Ulcerative colitis and colorectal cancer. A population-based study. NEJM 18; 323:1228-1233 (November 1, 1990).[2] Tsunozaki H, Yoshinaga K et al. Cyclooxygenase-2 Overexpression in Colorectal Cancer is Associated with Non-polypoid Growth. Japanese Journal of Clinical Oncology 32:167-171 (2002).[3] Eberhart CE, Coffey RJ, Radhika A, Giardiello FM, Ferrenbach S, DuBois RN: Up-regulation of cyclooxygenase 2 gene expression in human colorectal adenomas and adenocarcinomas. Gastroenterology 1994, 107(4):1183-8.[4] Lynch HT, de la Chapelle A. Hereditary Colorectal Cancer. NEJM 10;348:919-932. [5] Feik E, Baierl A. Association of IGF1 and IGFBP3 polymorphisms with colorectal polyps and colorectal cancer risk. Cancer Causes Control. 2010 Jan;21(1):91-7. [6] Ma, Jing, et al. Prospective study of colorectal cancer risk in men and plasma levels of insulin-like growth factor (IGF)-I and IGF-binding protein-3. JNCI, Vol. 91, April 7, 1999, pp. 620-25 [7] Hirayama K, Baranczewski P et al. Effects of human intestinal flora on mutagenicity of and DNA adduct formation from food and environmental mutagens. Carcinogenesis, Vol. 21, No. 11, 2105-2111, November 2000. © 2000. [8] Todar, K. The Normal Bacterial Flora of Humans. Online Textbook of Bacteriology. [9] http://www.sciencedaily.com/releases/2010/03/100309131752.htm [10] Roy M. Soetikno, MD, MS; Tonya Kaltenbach, MD, MS; et al. Prevalence of Nonpolypoid (Flat and Depressed) Colorectal Neoplasms in Asymptomatic and Symptomatic Adults. JAMA. March 5, 2008;299(9):1027-1035. [11] http://www.webmd.com/colorectal-cancer/news/20080306/flat-lesions-linked-to-colon-cancer [12] http://www.eurekalert.org/pub_releases/2008-12/acop-csr120908.php [13] http://www.nytimes.com/2008/12/16/health/16cancer.html?_r=1 [14] Lacy A, Garcia J et al. Laparoscopy-assisted colectomy versus open colectomy for treatment of non-metastatic colon cancer: a randomised trial. Lancet. 2002 Jun 29;359(9325):2224-9. [15] Skeel RT, ed. Handbook of Cancer Chemotherapy. 7th edition. © 2007, Lippincott Williams & Wilkins, Philadelphia, PA. ISBN 978-0-7817-6531-2. (page 271). [16] Oakman C, Pestrin M et al. Significance of Micrometastases: Circulating Tumor Cells and Disseminated Tumor Cells in Early Breast Cancer. Cancers 2010, 2(2), 1221-1235; doi:10.3390/cancers2021221. [17] Andrew Pollack, Therapies for Cancer Bring Hope and Failure. New York Times, June 14, 2010 [18] Saif MW. K-Ras mutations in colorectal cancer: A Practice Changing Discovery. Clinical Advances in Hematology & Oncology Volume 7, Issue 1 January 2009. [19] AS Baverman, Medical Oncology in the 1990s. The Lancet, Volume 337, Issue 8746, Pages 901 – 902, 13 April 1991 [20] Cristofanilli M, Budd T et al. Circulating Tumor Cells, Disease Progression, and Survival in Metastatic Breast Cancer. NEJM 351;824-26. [21] Molnar B, Ladanyi A et al. Circulating Tumor Cell Clusters in the Peripheral Blood of Colorectal Cancer Patients. Clinical Cancer Research (December 2001); 7: 4080-85. [22] Cristofanilli M, Budd T et al. Circulating Tumor Cells, Disease Progression, and Survival in Metastatic Breast Cancer. NEJM 351;824-26. [23] Raponi M, Winkler H, Dracopoli NC. K-RAS mutations predict response to EGFR inhibitors. Curr Opin Pharmacol. 20078;8:413-418. [24] Saif MW. K-Ras mutations in colorectal cancer: A Practice Changing Discovery. Clinical Advances in Hematology & Oncology Volume 7, Issue 1 January 2009. [25] ibid [26] www.orthomolecular.org/resources/omns/v01n09.shtml [27] National Cancer Institute, Mistletoe. Accessed at www.cancer.gov/cancerinfo/doc.aspx?viewid=1894c4cd-aa87-4f84-8ee4-9a815ce7f90e [28] R. G.-Maticek, Prof Dr med, H. Kiene, Dr med, et al; Use of Iscador, an extract of European mistletoe (viscum album), in cancer treatment: Prospective nonrandomized and randomized matched-pair studies nested within a cohort study. Alternative Therapies, May/June 2001, Vol. 7, no.3 [29] Ng K, Wolpin BM, et al; Prospective study of predictors of vitamin D status and survival in patients with colorectal cancer. British Journal of Cancer; September 15, 2009; 101(6):916-23 [30] Arber N. Cyclooxygenase-2 Inhibitors in Colorectal Cancer Prevention. Cancer Epidemiology, Biomarkers & Prevention August 2008 17; 1852. doi: 10.1158/1055-9965.EPI-08-0167. [31] Mantzoros CS, Williams CJ et al. Adherence to the Mediterranean dietary pattern is positively associated with plasma adiponectin concentrations in diabetic women. American Journal of Clinical Nutrition, Vol. 84, No. 2, 328-335, August 2006. [32] Barb D, Williams CJ et al. Adiponectin in relation to malignancies: a review of existing basic research and clinical evidence. Am J Clin Nutr. 2007 Sep;86(3):s858-66. [33] Baldwin C, Millette M et al. Probiotic Lactobacillus acidophilus and L. casei mix sensitize colorectal tumoral cells to 5-fluorouracil-induced apoptosis. Nutr Cancer. 2010 Apr;62(3):371-8. [34] Lieberman DA, Prindiville S, et al; Risk factors for advanced colonic neoplasia and hyperplastic polyps in asymptomatic individuals. JAMA., 2003 Dec 10;290(22):2959-67. [35] Garland CF, Comstock GW, et al; Serum 25-hydroxyvitamin D and colon cancer: eight-year prospective study. Lancet, 1989 Nov 18;2(8673):1176-8.Colon Cancer Overview
