 Patients ask me this question all the time. We diagnose the disease, we
treat with antibiotics, or herbs, or homeopathics. We feel better. We
stop the treatment. And either we continue to feel better, or we relapse
and have to start all over again.
Patients ask me this question all the time. We diagnose the disease, we
treat with antibiotics, or herbs, or homeopathics. We feel better. We
stop the treatment. And either we continue to feel better, or we relapse
and have to start all over again.
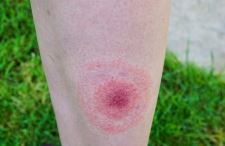 Is there no way to test whether the spirochete is gone?
Is there no way to test whether the spirochete is gone?
The Lyme disease.org website has an excellent article on diagnosis of Lyme disease.
The National Geographic website has a good description of the deer tick, and the history of Lyme disease.
Standard Lyme testing includes the following:
- ELISA or IFA test –
- If that test is positive, then a Western Blot test is run
- If 5 out of the 10 possible Lyme bands are positive, you are diagnosed with Lyme disease
- If fewer than 5 of the 10 possible bands are positive, you are diagnosed as negative.
Not all the bands which appear on a Western blot are specific to Lyme disease
– even though one of
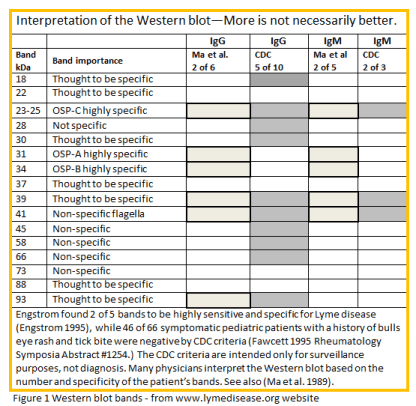 those non-specific bands is required by the CDC for diagnosis.
those non-specific bands is required by the CDC for diagnosis.
Two of the bands which are specific to Lyme disease are not on the CDC list of bands required to be positive.
How much sense does that make?
For more detailed information about the IFA and Western blot testing, check out the IGeneX website.
There is another test that can give us an idea whether the Lyme disease is actually gone out of our systems. This is an inflammatory marker, so it tells us whether there is continued inflammation (presumably caused by the Lyme bacterium) or whether that inflammation is no longer present.
This test is called “complement split products” – C3a and C4a may be early markers of Lyme disease and other inflammatory conditions like multiple sclerosis (which may be nothing more than the result of infection with the Lyme disease organism).
In one study, all early Lyme disease patients had higher C3a and C4a levels than the control group.[i] In another study, patients with chronic Lyme disease (and also patients with AIDS) had normal C3a levels but significantly elevated C4a levels. And response to antibiotic therapy resulted in a significant decrease in C4a levels, where lack of response was associated with an increase in those levels.[ii] This test is not specific to Lyme disease, but at least it is a decent measure of systemic inflammation.
In order for the spirochetes to survive in the bloodstream, they have to evade the complement proteins, which are like soldiers produced by the body to kill invading organisms. Many species of Borrelia are able to produce a complement regulator called Factor H which effectively hides them from the body’s complement soldiers.
It is as though the Factor H enables Borrelia to hide from the blood’s complement proteins in plain sight.[iii] The complement is struck blind, and can no longer “see” the Borrelia organisms. More and more complement is produced, in an effort to improve its effectiveness, to no avail if the organisms are not destroyed somehow – whether by the body’s own immune defenses, or by antibiotics.
Borrelia also appear to express a protein called decorin on its surface. Decorin-protected organisms are much more infectious than organisms which do not express decorin. A monoclonal antibody called GB6 has been manufactured, active against decorin. It protects mice very nicely, but it has not yet been made available for human use.[iv]
Bottom line:
- there are better Western blot tests than the ones used by conventional laboratories.
- There are tests of inflammation at least a little bit specific to progression (or regression) of Lyme disease
- It may be possible to determine whether Lyme disease has been treated effectively by using the tests of inflammation
There is hope for more accurate and adequate testing of this miserable affliction, and there is even hope for treatment.
Call us if you are looking for effective treatment of Lyme disease. Depending on the stage of infection, and how well you can function, we have a variety of treatment programs which can help you heal.
[i] Shoemaker RC1, Giclas PC, Crowder C, House D, Glovsky MM. Complement split products C3a and C4a are early markers of acute lyme disease in tick bite patients in the United States. Int Arch Allergy Immunol. 2008;146(3):255-61. doi: 10.1159/000116362
[ii] Stricker RB1, Savely VR, Motanya NC, Giclas PC. Complement split products c3a and c4a in chronic lyme disease. Scand J Immunol. 2009 Jan;69(1):64-9. doi: 10.1111/j.1365-3083.2008.02191.x.
[iii] Kraiczy P, Skerka C, Kirschfink M, Brade V, Zipfel PF. Immune evasion of Borrelia burgdorferi by acquisition of human complement regulators FHL-1/reconectin and Factor H. Eur J Immunol. 2001 Jun;31(6):1674-84.
[iv] Liang FT, Brown EL, Wang T, Iozzo RV, Fikrig E. Protective niche for Borrelia burgdorferi to evade humoral immunity. Am J Pathol. 2004 Sep;165(3):977-85.
