As of April 1, 2015, the CDC reports[1]there were 719,000 total knee replacements in the United States, and 332,000 total hip replacements.

In 2014, the Mayo Clinic reported that 4.7 million Americans have had knee replacement surgery; 2.5 million have had hip replacement surgery – more women than men.[2] Their point was that the replacement surgery helped these patients to stay mobile. They did not present evidence of mobility, just that a lot of people were living with artificial joints in the United States.
A Japanese study published in 2010 followed 41 patients for 11 years after bone marrow-derived mesenchymal stem cell transplantation for cartilage repair. The patients were initially treated in 1988. None of the patients had developed tumors or infections in all that time. The abstract did not discuss how mobile the patients were after 11 years, but it did emphasize the safety of the procedure.[3]
According to Healthline, a provider of health information and technology solutions headquartered in San Francisco, the average charge for in-hospital total knee replacement in the USA is $57,000. There are additional charges for pre- and post-hospitalization visits and physical therapy. Typically Medicare pays for around 80% of these charges, leaving the average patient with over $11,000 in out-of-pocket costs.
You will be pleasantly surprised to learn that the average out-of-pocket cost for stem cell therapy in the United States is about $7500, including pre- and post-procedure visits and follow-up.
Curiously, stem cell therapy is still considered experimental, since it was first reported by the Japanese in 1988 – twenty-seven years ago. One wonders how long it will take before this form of therapy is considered standard of care, rather than experimental.
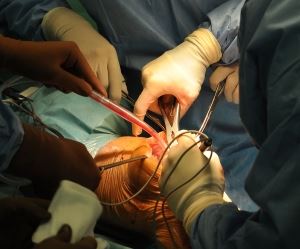 Arthroscopic knee surgery shows no particular long-term benefits, as reported
in the British Medical Journal in 2015.[4] Initial benefits are limited to a small decrease in pain, and no benefit
in physical function. These benefits were limited to the first 6-12 months,
and appeared to vanish within one or two years of the surgery. Adverse
effects of the procedure included deep vein thrombosis (blood clots in
the legs), pulmonary embolism (blood clots traveling from legs to lungs)
and even death.
Arthroscopic knee surgery shows no particular long-term benefits, as reported
in the British Medical Journal in 2015.[4] Initial benefits are limited to a small decrease in pain, and no benefit
in physical function. These benefits were limited to the first 6-12 months,
and appeared to vanish within one or two years of the surgery. Adverse
effects of the procedure included deep vein thrombosis (blood clots in
the legs), pulmonary embolism (blood clots traveling from legs to lungs)
and even death.
A Japanese group reported in 2014 both a phase I study for safety and a phase II study for efficacy of stem cell injection treatment for injured knee joints with cartilage defects. There were no treatment-related adverse events. The pain and function scores improved at 6 months, and the size of the cartilage defect decreased. The new cartilage appeared to be normal when examined under the microscope.[5]
Twenty-seven years ago the procedure was both safe and effective. In 2014 the procedure is again reported to be both safe and effective.
What are we waiting for? This form of therapy can be available in your physician’s office. It is safe, and effective, and cost-effective. But not covered by insurance since, after 27 years, it is still considered to be “experimental”.
Call the Arizona Center for Advanced Medicine to schedule a free 15-minute phone consultation with one of our practitioners, to discuss the possibility of effective forms of cell therapy for chronic knee, hip or shoulder joint pain and arthritis. You may be able to save yourself a trip to the operating room.
[2] Prevalence of Total Hip (THA) and Total Knee (TKA) Arthroplasty in the United States. P001-P110-Adult Reconstruction Hip Posters, 03-11-14, presentation # P057.
[3] Wakitani, S., Okabe, T., Horibe, S., Mitsuoka, T., Saito, M., Koyama, T., Nawata, M., Tensho, K., Kato, H., Uematsu, K., Kuroda, R., Kurosaka, M., Yoshiya, S., Hattori, K. and Ohgushi, H. (2011), Safety of autologous bone marrow-derived mesenchymal stem cell transplantation for cartilage repair in 41 patients with 45 joints followed for up to 11 years and 5 months. J Tissue Eng Regen Med, 5: 146–150. doi: 10.1002/term.299
[4] Thorlund JB, Juhl CB, Roos EM, Lohmander LS. Arthroscopic surgery for degenerative knee: systematic review and meta-analysis of benefits and harms. Br J Sports Med. 2015 Oct;49(19):1229-35. doi: 10.1136/bjsports-2015-h2747rep.
[5] Jo CH, Lee YG et al. Intra-articular injection of mesenchymal stem cells for the treatment of osteoarthritis of the knee: a proof-of-concept clinical trial. Stem Cells. 2014 May;32(5):1254-66. doi: 10.1002/stem.1634.
