Republished with permission from EXPLORE! Publishing, 928 541-1920
or 800 320-6035, P.O. Box 11510, Prescott, AZ 86304
Cancer cells are different than healthy cells. For one, they use a lot more sugar. For another, they give off a lot more heat.
Chemical and blood vessel activity in the area surrounding a developing breast cancer is almost always higher than in the normal breast. Cancer cells need an abundant supply of nutrients to maintain their growth and this increased blood flow can increase the surface temperatures of the breast. When a tumor is forming, it develops its own blood supply to feed its accelerated growth, a process known as malignant angiogenesis. Pre-cancerous tissues can start this process well in advance of the cells becoming malignant.
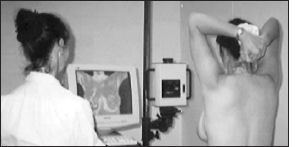 Thermography measures the skin’s autonomic response to that inflammation
– its “heat signature”.
Thermography measures the skin’s autonomic response to that inflammation
– its “heat signature”.
The technology converts infrared radiation emitted from the skin surface into electrical impulses that are visualized in color. The spectrum of colors indicates an increase or decrease in the amount of infrared radiation being emitted from the body surface.
Professionals look for asymmetry in the heat pattern. In other words, how might one breast differ from another?
 |
 |
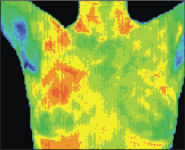 |
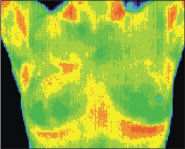
| Baseline | 3 Months | 6 Months |
 |
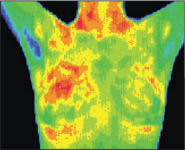
9 Months |
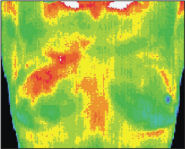
12 Months |
 |
This patient was age 37 when her first baseline thermogram showed a slight hyperthermic asymmetry in the upper right breast. The follow-up 3 months later shows the pattern had become more well defined. A third thermogram shows significant changes. Mammography was performed at this stage; the mammographic findings were inconclusive. The fifth comparative thermographic study at 12 months shows the temperature differential (hyperthermic asymmetry) has increased.
A repeat mammogram was performed which clearly showed a small calcification (1 mm) at one o’clock. Within one week a lumpectomy had been performed with good margins and the pathology confirmed as a malignant carcinoma (DCIS). [1]
The August 2007 issue of Radiology bemoans the growing number of mammography centers across the United States that are closing down. Radiologists blame low reimbursement from the insurance companies and a frightening degree of liability.
With mammograms, the false negative reading rates (not detecting cancers) range from 10% to 40%.
According to the 2002 Breast Cancer Study, issued by the Physician Insurers Association of America (PIAA), internists were named in 7% of the surveyed failure-to-diagnose breast cancer suits brought during the 1990s. Family physicians were named in 11% of cases and gynecologists in 29%. Radiologists topped the list, however, being named in 40% of all failure-to-diagnose breast cancer claims.
That observation has not been lost on future generations of radiologists, many of whom are avoiding mammography.
Mammography has not proved to be a flawless screening tool. It has a difficult time giving a good reading in women with dense breasts. It exposes women year after year to radiation. As every woman knows who has undergone one, it hurts to have breast tissue squished between two pieces of metal. And there is the argument that compressing cancerous tissue will just spread the malignancy.
Researchers have long warned that the compressive force used to obtain useable mammograms may be a contributing factor to breast cancer:
The British standard for the force used to squeeze the breast as flat as possible corresponds to placing twenty 1 kilogram bags of sugar on each breast. Researchers [at the University of Aberdeen, Scotland] fear that this force may be excessive and enough to dislocate and spread any existing cancer cells. Animal experiments have shown that the number of cancer sites can increase by as much as 80% when tumors are manipulated mechanically. A recent study in Malmo, Sweden found that the death rate from breast cancer among women under 55 was 29% higher in a group which had been screened with mammography than in the unscreened control group. [2]
There is mounting evidence that the x-rays from repeated mammograms induce cancer. Dr. John W. Gofman, an authority on the health effects of ionizing radiation, estimates that 75 percent of breast cancer could be prevented by avoiding or minimizing exposure to the ionizing radiation. This includes mammography, x-rays and other medical and dental sources. [3]
“Since a mammogram is basically an x-ray (radiation) of the breast, I do not recommend mammograms to my patients for two reasons: 1) Few radiologists are able to read mammogams correctly, therefore limiting the procedure’s effectiveness. Even the man who developed this technique stated on national television that only about six radiologists in the United States could read them correctly. 2) In addition, each time the breasts are exposed to an x-ray, the risk of breast cancer increases by 2 percent.” [4]
What other options are there?
Digital mammography is a mammography system in which x-ray film is replaced by solid-state detectors that convert x-rays into electric signals. Radiologists find that, like mammograms, it also produces many false positives.
Breast magnetic resonance imaging (MRI) is another option. In younger women, this approach offers two advantages: the lack of ionizing radiation and the capability for enhanced imaging of dense breasts. However, this mode has a very high false-positive rate, is expensive, and requires specialized apparatus should a biopsy be necessary.
Thermography is a non-invasive, fifteen minute test. It does not use radiation, does not compress breast tissue, and it is better than mammography at early detection of breast function abnormalities. It has a lot going for it. So why is thermography not more widely practiced?
Thermography debuted in the 1970s as a modern technique, but it was actually first mentioned by Hippocrates in 480 BC. A slurry of mud was spread over the patient. Those areas which dried first were presumed to be “hot” and to indicate pathology of the organs underlying them. In the 1800s, William Herschel was the first to recognize that “dark heat” was emitted and that it behaved like light, could be both reflected and refracted under the right circumstances. His son, John, made an image using solar radiation, focusing the sun’s rays onto a suspension of carbon particles in alcohol. He called this image a “thermogram”. Sensitive healers have been able to detect this heat signature using their own body sensors for thousands of years.
In the 1950s, the military began to use infrared monitoring systems to follow night time troop movements. In 1956, Ray Lawson, MD published a brief article describing a thermocouple device which he used in cases of suspected breast cancer as a diagnostic tool. He found an increased temperature signature of between 3.5º and 1.3º in a series of patients with subsequently proven breast cancer. [5]
When the technology was in its infancy, “eyeballing” the images was the only way to detect abnormalities or asymmetries, and controls and protocols were not always followed. It is little surprise, then, that an article published in CA, A Cancer Journal for Clinicians, concluded, “We have found little evidence to indicate that clinical thermography lowers the stage at detection, and neither does a positive thermogram in screening seem to have a strong predictive value.” [6] When the thermogram was thought to have given a “false positive”, in other words, the thermogram was positive but no tumor was found, this finding was interpreted to mean that the test was inaccurate.
These early researchers were looking for a tool which would be capable of diagnosing breast cancer. What they apparently failed to realize is that thermography will never be capable of diagnosing breast cancer – that it is only under the microscope that cancer can actually be diagnosed. Thermography is a functional test, measuring a heat signature produced by increased vascularity. This may be due to cancer, but it may also be due simply to inflammation without cancer. Mammography cannot diagnose cancer either – it can only diagnose a physical or structural abnormality. The advantage of the thermogram is that we can measure inflammation at an early stage – perhaps even before cancer (a disease of inflammation) has a chance to develop.
In 1972, a position paper was published by the Department of Health, Education and Welfare, in which was stated that thermography was a viable method as a diagnostic procedure in the area of pathology of the human breast. In 1982, the FDA published its approval and classification of thermography as an adjunctive diagnostic screening procedure for the detection of breast cancer.
In the 1990s, significant work was done by the military, in an effort to translate their work with infra-red imaging into the medical field. [7,8]
The Breast Cancer Detection and Demonstration Project (BCDDP) is a multi-center study performed from 1973-79, and was aimed at demonstrating whether thermography could replace mammography or breast examination as a sole screening tool. Unfortunately, there were significant protocol violations, environmental controls were ignored, and many of the personnel who collected the data were untrained in thermography technique, in addition to which there were no established reading protocols. Thus the data collected were poor, many of the images were unreadable, and interpretations were seriously open to question.
The more thermograms turned in so-called false positives, the more suspicion was placed on thermography. Although a decade later many of those “false positive” women were found to have developed breast cancer, the establishment had already spoken, declaring thermography a failure.
Meanwhile, the insurance industry had turned against thermography as well. It is tempting to speculate that it was because juries could clearly see the physiological component of pain and injury due to car accidents, job injuries, and a host of other tort related law suits, making it somewhat more difficult to deny claims related to stress injury.
Eventually, lobbying efforts at the American Medical Association’s House of Delegates and at Medicare, brought about the removal of thermography coverage by insurance companies. Thermography was viewed as a competitive tool to mammography. To this day, the American Cancer Society still promotes only mammography.
International writings on the subject ask questions about mammography that we do not see in the American press.
The major, surprising finding of the Canadian National Breast Screening Study was that there is no evidence that screening for breast cancer with mammography is effective for women under 50 years of age. Not surprisingly, this conclusion has been vehemently attacked by American radiologists. Women in their 40s are the best customers for regular mammograms. As many as 40% of them have an annual mammogram at a cost of $50-100 each. Now another study in Sweden supports the Canadian findings. Dr. Lazlo Tabar followed 35,000 women aged 40-49 for 11 years. He found no evidence that regular mammographic screening of these women had any benefits. [9]
A large study of the benefits of mammography screening for breast cancer was carried out in 2001 by the prestigious Cochrane Institute. The study questioned the benefits of screening and pointed out that screening could be harmful in that it frequently leads to over-diagnosis and over-treatment. The Cochrane Institute has now released the results of a new study aimed at determining how fairly the benefits and dangers of mammography are presented on web sites. They evaluated 13 sites maintained by advocacy groups, 11 maintained by governmental institutions, and 3 maintained by consumer organizations. They found that all the advocacy group sites accepted sponsorship from industry without restriction. The close relationship can perhaps best be summed up in this quote from the Canadian Cancer Society, “Partnership with the Canadian Cancer Society can assist your company in reaching your commercial objectives.” The researchers found that all the governmental agencies and advocacy groups heavily favoured screening and significantly downplayed the drawbacks; the consumer health organizations took a much more balanced view. [10]
Recent advances in technology have brought thermography to the point where it is now used as one of the diagnostic tools in two cancer research centers in North America. Today, there are very strict protocols both for testing and interpreting. Perhaps due to these guidelines, thermography (unlike digital mammography) has exploded in its technique and capabilities.
The consensus among experts is that early detection of breast cancer holds the key to survival. If mammography’s look at structure can detect a cancerous mass, and thermography’s look at systems can detect early suspicions of cancer formation, then it stands to reason thermography can act as an early warning system, giving women the fighting chance they need to win this battle.
Thermography is ideal for women who
- have had cosmetic or reconstructive surgery (implants)
- want to avoid radiation
- have dense breasts
- are pregnant or nursing
Screening – whether by thermogram, mammogram or any other means – is not diagnosis. Both thermography and mammography demonstrate abnormalities indicating the possibility of the presence of cancer, as well as a host of other breast conditions. These clinical findings require differential diagnosis. Only confirmation of abnormal cell morphology under the microscope can make the definitive diagnosis of cancer.
Neither thermography nor mammography has 100% accuracy. For that matter, physical diagnosis (palpation of the breast) is not 100% accurate either. These tests are the best we have. Any effective tool which does not traumatize the breast or deliver ionizing (mutating) radiation is far preferable as a screening tool to one which causes damage while it is screening.
Thermography is useful for evaluating other parts of the body as well. Thermography is an excellent tool in sports medicine and pain management because it can map inflammation from neurologic or musculoskeletal dysfunction. It can also be of assistance in the evaluation of deep vein thrombosis, insufficiency of the blood supply, and more. We can even see changes in the area of the abdomen which could indicate inflammatory bowel disease like colitis, ileitis or Crohn’s disease.
A brief word about cancer:
Cancer is brought on by inflammation, which may be triggered by trauma.
That trauma can take different forms
- Emotional – such as feelings of unworthiness relating to one’s femininity
- Mental – such as our mindset about shame that create ongoing brain patterns that manifest physically
- Physical – such as a car accident, or other direct trauma to the breast
A thermogram which has only “inflammatory” change should prompt further testing in the form of a mammogram. No matter what the mammogram shows, negative or positive, holistic preventive care is appropriate. The patient is encouraged to visit a practitioner of holistic medicine who can help reduce the inflammation and possibly head the problem off at the pass. Inflammatory change will never be seen with mammography, because it only sees anatomy, not function. A negative mammogram in the face of a positive thermogram suggests only that cancer has not developed yet, there is still time for preventive care.
Most cancers are in the body for up to 20 years before they become large enough to see with our crude methods of testing. Let us not waste those 20 years by hiding our heads in the sand. Let us spend them actively seeking healthful practices, excellent nutrition, and adequate exercise. Let us encourage the removal of all toxins from the body – cigarettes, alcohol, drugs, pharmaceuticals, worry, anxiety, resentment and fear. And, above all, let us practice gratitude, that our lives may be abundantly full and joyful. Then inflammation will decrease on all levels, and health will be restored.
“But breast cancer runs in my family, so I will get it too.” Not necessarily. If trauma, stress, and lack of good nutrition culminate in disease, then where is the weak spot? Where is the body most likely to break down? If breast cancer runs in the family, then indeed, a person may develop breast cancer. If arthritis, another inflammatory immune system disorder, runs in the family, another person may develop joint problems instead. If a person takes better than average care of herself, mentally and physically, she may not fall prey to breast cancer even though it runs in the family. There may be an inherited a pre-disposition, but that does not necessarily mean that it will develop.
The Susan G. Komen Foundation funded a study released in May, 2007, that essentially found that our increasingly polluted and toxic environment is much to blame for the rise in cancer. As reported in the press: [11]
More than 200 chemicals – many found in urban air and everyday consumer products – cause breast cancer in animal tests, according to a compilation of scientific reports published today.
Writing in a publication of the American Cancer Society, researchers concluded that reducing exposure to the compounds could prevent many women from developing the disease.
The research team from five institutions analyzed a growing body of evidence linking environmental contaminants to breast cancer, the leading killer of U.S. women in their late 30s to early 50s.
Experts say that family history and genes are responsible for a small percentage of breast cancer cases but that environmental or lifestyle factors such as diet are probably involved in the vast majority.
In other words, environmental toxins continually pollute the body. Our natural detoxification systems work less efficiently over time. More free radicals are formed, damaging our DNA. The stage is set for disease.
Thermography is a screening tool which can help raise suspicions of breast cancer at an early stage, when there is still chance of complete cure.
Established patients can simply call to make an appointment for a thermogram. New patients who wish to have thermography are evaluated medically first, before having the test. Other patients may be referred just for a thermogram by their regular physician, to whom we will send a report.
Q & A
Q – How can thermography detect potential cancers so many years earlier than mammography?
A – When a tumor is forming, it develops its own blood supply to feed its accelerated growth, a process known as malignant angiogenesis. Pre-cancerous tissues can start this process well in advance of the cells becoming malignant.
Q – You recommend that if the thermogram suggests cancerous tissue may be present, that one follow up with a mammogram. Why?
A – Because thermography is a functional test, mammography is an anatomic test. If the functional test is suspicious, then you want to look at the anatomy. Often times, thermography catches breast cancer sooner than it can be felt by palpation. Mammography can look for a mass that is still too small to be felt. Even mammography considers a “small” tumor to be 2 cm in diameter (1 inch = 2.5 cm), which is a large mass of cells. So if we see something suspicious on a thermogram, the risk of x-rays and compression is a risk worth taking , because we may be able to see a much smaller tumor. Using mammography in this way means exposing yourself to x-rays and compression only when absolutely necessary, rather than routinely year after year.
Q – What happens during the test?
A – For instructions on how to prepare for a thermography exam, click here.
[1] American College of Clinical Thermography. Accessed August 2007 at http://www.thermologyonline.org/breast_thermography_procedure.htm[2] The Lancet, July 11, 1992, p. 122[3] John W. Gofman, M.D., Ph.D., Radiation from Medical Procedures in the Pathogenesis of Cancer and Ischemic Heart Disease, C.N.R. Book Division, Committee for Nuclear Responsibility, Inc., San Francisco, 1999[4] Francisco Contreras, MD; The Hope of Living Cancer Free, Creation House, 1999, page 104[5] Lawson R. Implications of Surface Temperatures in the Diagnosis of Breast Cancer. Canad MAJ 75:309-310 (Aug 15, 1956).[6] Moskowitz M. Screening for Breast Cancer: How Effective Are Our Tests? A Critical Review. CA Cancer J Clin 1983;33:26039.[7] Diakides NA. Medical Applications of IR Focal Plane Arrays, – Final rept. Advanced Concepts Analysis Inc Falls Church Va. NTIS report # ARO-32870.1- EL-S.[8] Paul JL, Lupo JC. From tanks to tumors. Engineering in Medicine and Biology Magazine, IEEE 21;6:34-36 (Nov-Dec 2002).[9] Charlotte Gray, US resistance to Canadian mammogram study not only about data, Canadian Medical Association Journal, Vol. 148, No. 4, February 15, 1993, pp. 622-23[10] Jorgensen, KJ and Gotzsche, PC. Presentation on websites of possible benefits and harms from screening for breast cancer: cross sectional study. British Medical Journal, Vol. 328, January 17, 2004, pp. 148-53[11] Marla Cone, Common chemicals are linked to breast cancer, Los Angeles Times, May 14, 2007